Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
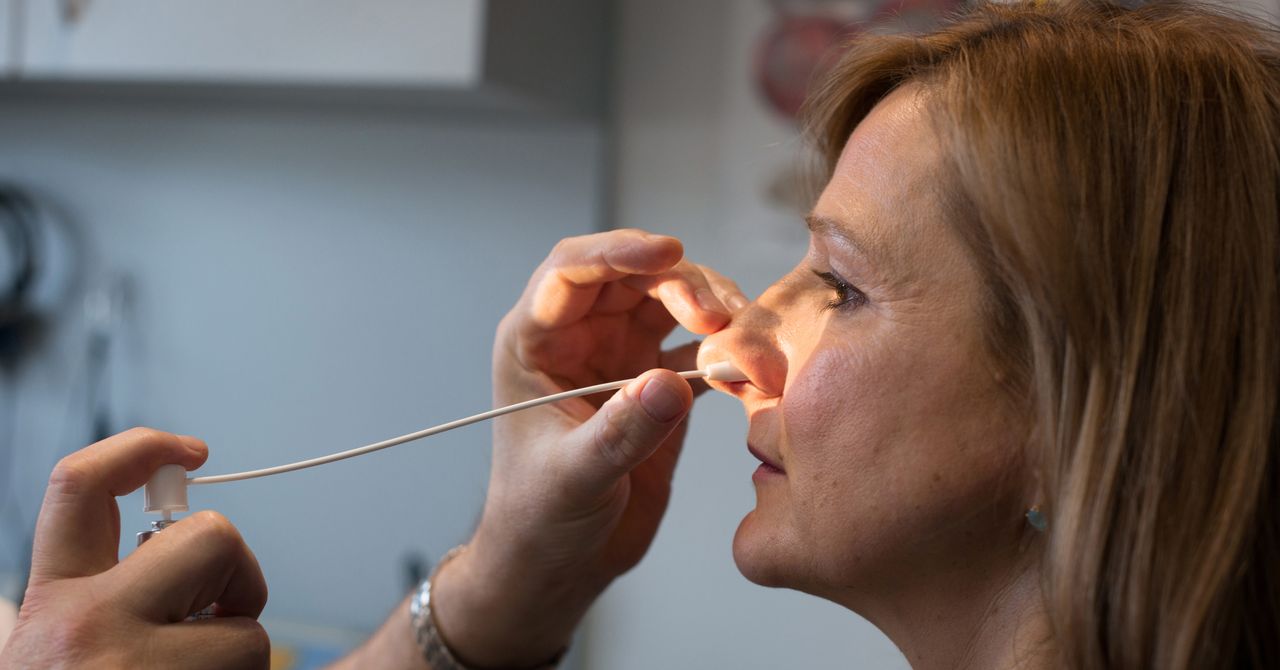
Middle-aged, women They were told to expect turmoil. Sleep may become lighter, nights may feel warmer, and energy may become more difficult to obtain. Hormones change, and the body adapts. But for many women, something else is going on as well: their airways collapse dozens of times an hour during pregnancy He sleeps.
Disabled Sleep apnea OSA, once classified as a disorder primarily affecting older, heavier men, is increasingly recognized as a more complex and often undetected condition, especially in premenopausal women and menopause.
Obstructive sleep apnea (OSA) occurs when the upper airway narrows or collapses during sleep, oxygen levels drop, and the brain briefly wakes the body to restart breathing. For years it has been framed as a single disorder with a familiar face. Now researchers understand it to be much more complex: a heterogeneous condition shaped by different biological mechanisms and expressed through different symptom patterns. However, the archetype of older, larger males continues to shape who is diagnosed and who is not.
Modern Projection The Lancet Respiratory Medicine journal suggests that the problem is much bigger — and more female — than previously thought. Researchers estimate that by 2050, approximately 77 million American adults ages 30 to 69 will suffer from sleep apnea, including a 65 percent relative increase in its prevalence among women, to about 30.4 million, compared to a 19 percent relative increase among men. This increase reflects an aging population and rising obesity rates, but is also hopefully something more fundamental: better detection.
While more than a billion people in the world suffer from sleep apnea, up to 90 percent in some countries go undiagnosed and untreated, explains Carlos Nunez, chief medical officer at ResMed, which supported the analysis. “It’s a condition that often lives in anonymity. Most people don’t realize they have it, because you’re asleep when it happens,” he says.
Although OSA can appear at any age — even in children — the risk of developing it is higher, because decreased muscle tone makes it difficult for the airway to stay open during sleep. However, for women, menopause is a pivotal moment. Studies show that postmenopausal women have a much higher risk of developing obstructive sleep apnea (OSA). one analysis A US health survey found that postmenopausal women were 57 percent more likely to report symptoms of sleep apnea than premenopausal women, even after adjusting for body weight.
“Women have hormonal protection from estrogen until menopause,” says Marie-Pierre St. Onge, director of the Center of Excellence for Sleep and Circadian Research at Columbia University. At that time, fat distribution shifts toward the neck and upper body, which increases pressure on the airway, she explains.
research suggests Estrogen and progesterone have protective effects on the regulation of breathing and upper airway muscle activity. As hormone levels decline after menopause, this effect diminishes, which may contribute to an increased likelihood of airway collapse during sleep.
Rashmi Nisha Aurora, MD, professor of medicine and director of the Women’s Sleep Medicine Initiatives at NYU Grossman School of Medicine, describes estrogen as a master antioxidant. When it decreases, protection against oxidative stress is weakened, just as OSA itself exposes the body to frequent oxygen drops and inflammatory stress. The result, she argues, is a physiological “double whammy” that increases stress on the heart and metabolic system.
Aurora notes that pregnancy is another time when hormonal fluctuations temporarily increase susceptibility to sleep apnea.
The irony is that menopause also occurs when obstructive sleep apnea (OSA) is easier to explain, as symptoms in women — which can differ from those in men — include night sweats, fatigue, and restless sleep, which overlap with menopause itself. “This is where it really gets overlooked,” says Aurora. “Part of the problem was identifying the case and examining it.”
The checklists that clinicians rely on—loud snoring, marked apnea, and excessive daytime sleepiness—were developed and validated largely in all-male or mixed-gender populations. Many of the tools most commonly used to measure hypersomnia, including the Epworth Sleepiness Scale, have not been validated in women across age groups. Symptoms that often lead to CPAP referral may be such as excessive daytime sleepiness described Or a different experience by women.