Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
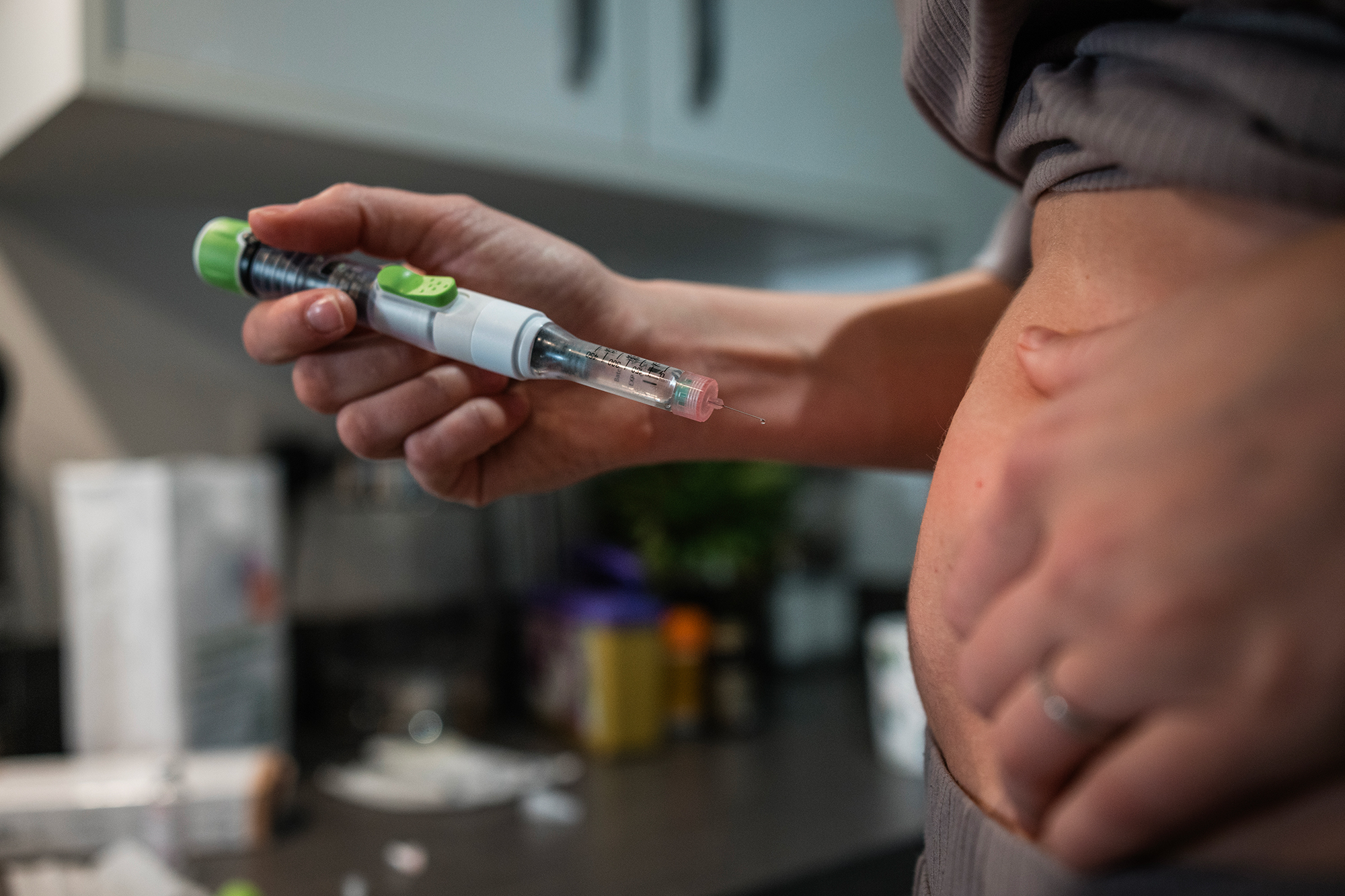
from Kristen HuangCalMatters
This story was originally published by CalMatters. Sign up for their newsletters.
Like many young girls, Mara Burton and June Higginbotham knew from an early age that they wanted families and to become mothers. But as lesbians, they were excluded from accessing the same fertility treatment insurance benefits offered to their heterosexual peers.
Instead, like many other same-sex couples, Burton and Higginbotham, who live in Santa Clara County, had to pay $45,000 out of pocket to conceive, while heterosexual counterparts with the same insurance plan covered many of those costs.
“We knew it wasn’t right,” Berton said in an exclusive interview with CalMatters. She joined a class action lawsuit challenging the policy. “What we’re fighting for is building a family and having children… I think it was very important to both of us that other couples don’t have to do that.”
Last week, in a landmark settlement, U.S. District Judge for the Northern District of California Haywood Gilliam Jr. approved prior agreement for the class action requiring Aetna to cover infertility treatments for same-sex couples — such as artificial insemination or IVF — as they do for heterosexual couples. This is the first case requiring a health insurer to implement this policy nationally for all of its participants. An estimated 2.8 million LGBTQ members will benefit, including 91,000 Californians.
Under the settlement, Aetna will also pay at least $2 million in compensation to California-based members who qualify. Those who can qualify should file a claim by June 29, 2026.
“I really hope this is the first of many insurers to change their policies,” said Alison Tanner, senior counsel for reproductive rights and health litigation at the National Women’s Law Center. “We saw it as an inequality issue – that people who were in same-sex relationships were treated differently.”
An estimated 9 million additional Californians will soon have access to compulsory maternity benefits under a new law that goes into effect in January. The law applies to state-regulated plans — which Aetna is not in this case — and changes the definition of infertility to include same-sex couples and single people.
Previously, Aetna’s policy required enrollees to engage in six to 12 months of “unprotected heterosexual intercourse” without conceiving before qualifying for fertility benefits, according to class action complaint. The policy allowed women “without a male partner” to access benefits only after six to 12 unsuccessful IVF cycles, depending on age.
Advocates argued that the policy treats LGBTQ members differently and effectively denies them access to the benefit, which can be prohibitively expensive for many.
In an email, Aetna spokesman Philip Blando said the plan provides infertility benefits in accordance with each member’s plan, coverage rules and applicable law.
“Aetna is committed to equal access to infertility and reproductive health coverage for all of its members, and we will continue to strive to improve access to services for our entire membership,” Blando said.
Burton, who was the lead plaintiff in the case, said she was blindsided by politics. She had consulted with an infertility clinic and had decided to move forward with donor sperm and artificial insemination when a representative from Aetna called and said she did not meet the definition of infertility.
She appealed the decision multiple times; she was rejected. The experience felt “dehumanizing,” said her wife, Higginbotham.
Insurance had dictated that Burton try 12 cycles of artificial insemination before becoming eligible for benefits. Her doctors recommended no more than four rounds.
Sean Tipton, chief advocacy and policy director for the American Society for Reproductive Medicine, said such a policy could only be designed to dissuade people from accessing their health benefits. doctors usually recommend three to four cycles of artificial insemination before IVF, but Tipton said there are also studies that show it’s more effective and cost-effective to go straight to IVF.
In 2023, the society updated its medical definition of infertility to include LGBTQ people and people who don’t have partners. They did this in part to prevent insurers from rejecting claims like Burton’s and Higginbotham’s.
“The driving force was the realization that it takes two types of gametes to have children,” Tipton said. “Regardless of the reason for this absence, you must have access to treatment for a fertility problem.”
Since the definition changed, Tipton said more employers and insurers are covering benefits for LGBTQ people or single people. They’ve also used the definition to enact statewide benefits expansions, including California’s upcoming mandate for maternity benefits.
Burton and Higginbotham said they also worry about running out of donor sperm that matches Higginbotham’s Jewish and Native American heritage — and is in limited supply.
“I don’t think your insurance should be involved in these types of decisions and dictate your trip,” Berton said.
The couple raised money from family members and decided to continue even without coverage. After four unsuccessful rounds of IUI, they switched to IVF, in part to ensure the best chance of conceiving with the donor they chose.
The experience was “all-consuming” and emotionally difficult as Burton endured hormone injections, egg retrieval and a miscarriage. But today, she and Higginbotham have two healthy twins whose favorite thing is to play on the swings and “pull every book off the shelf” for their mothers to read.
The couple achieved their marital dreams before the case closed. Still, Higginbotham said she hopes the settlement will help other LGBTQ couples across the country.
“I know people who don’t have kids who wanted kids because things weren’t covered. I know people whose schedule was messed up and maybe they have fewer kids than they wanted,” Higginbotham said. “The agreement is such a huge step forward that really righted a huge mistake.”
Supported by the California Health Care Foundation (CHCF), which works to ensure that people have access to the care they need, when they need it, at a cost they can afford. Visit www.chcf.org to learn more.
This article was originally published on CalMatters and is republished under Creative Commons Attribution-NonCommercial-No Derivatives license.