Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
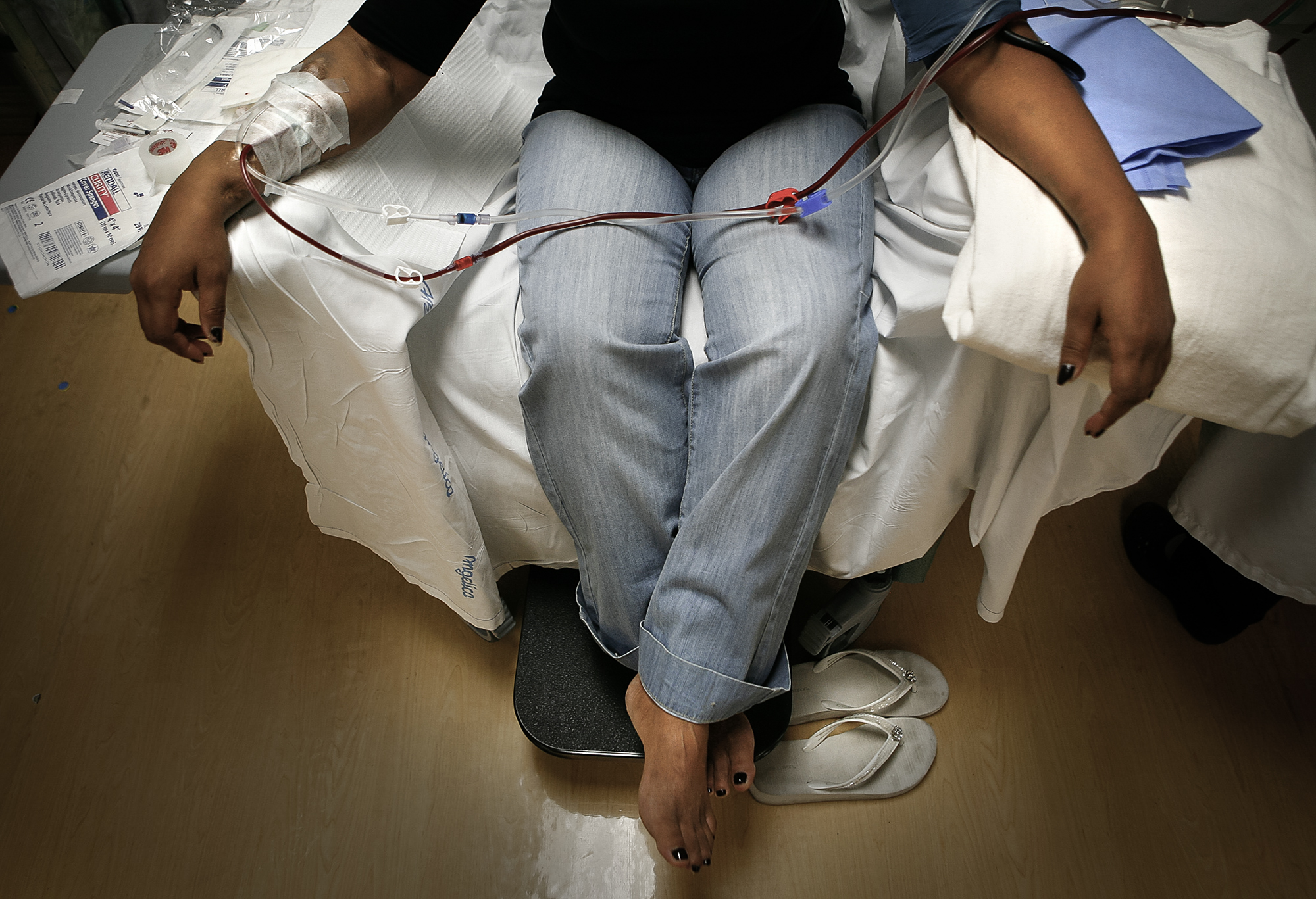
from Ana B. IbarraCalMatters
This story was originally published by CalMatters. Sign up for their newsletters.
A federal appeals court ruled last week that California’s attempt to cap dialysis companies’ profit from certain privately insured patients is unconstitutional — a victory for an industry that has repeatedly rebuffed efforts to control its costs.
9th US Circuit Court of Appeals struck key parts of Assembly Bill 290a law designed to limit how much dialysis companies can profit from privately insured patients who receive premium care from charitable groups.
About 800,000 people in the U.S. suffer from end-stage kidney disease, a condition that requires being connected to machines that filter their blood for up to five hours several times a week.
Most dialysis patients — about 80 percent — are on Medicare. But when patients end up on private insurance instead, costs rise. Individual market plans pay roughly three times what Medicare pays for dialysis, according to a 2021 study from the University of Southern California. Although dialysis patients make up only a small portion of the individual market, their average monthly costs are 33 times higher than those of other enrollees — driving up premiums for everyone else.
“The problem is that dialysis care is significantly more expensive in the individual market, and that has to do with how consolidated the market is,” said Dr. Eugene Lin, assistant professor of medicine at USC and co-author of the study.
At the center of the legal dispute was an alleged practice that supporters of the law called a “profit-maximizing scheme.” Dialysis providers DaVita Inc. and Fresenius Medical Care are donating to the American Kidney Foundation, a nonprofit organization that provides first-class care to about 3,000 dialysis patients in California. For years, insurers, consumer groups and unions have argued that, in exchange for those donations, the American Kidney Foundation steers patients away from public insurance — Medicare and Medicaid — and into private insurance by paying their premiums. This benefits dialysis providers because private insurance tends to pay higher rates than public payers. The American Kidney Foundation has long denied the allegations.
Lawmakers drafted AB 290, which Gov. Gavin Newsom signed in 2019, to target this alleged practice. First, it limited the reimbursement rate that dialysis providers could receive for privately insured patients who receive premium care from nonprofit charities. The law caps the reimbursement of what Medicare pays. It also requires those charities to disclose the names of patients who receive a premium so that insurers can know which patients are capped for reimbursement.
DaVita and Fresenius, along with the American Kidney Foundation and a patient group, sued the state soon after the law was passed, blocking it from taking effect.
Last week, the 9th Circuit ruled those provisions unconstitutional. The court found that the law’s reimbursement cap and patient disclosure provisions violated the First Amendment by burdening the American Kidney Foundation’s right to associate with DaVita and Fresenius. If California’s intent was to protect patients from malpractice and prevent distortion of the insurance risk pool — something that happens when health plans take on more high-cost patients — the state did not narrowly tailor the law’s provisions to achieve those interests, the justices said.
A district court previously struck down a separate provision of the law that more directly prohibited clinics from referring or advising patients about insurance plan options. The court said California did not provide enough evidence to support its argument that the charities or clinics were referring patients.
The appeals court’s decision drew praise from the industry. DaVita said he was “encouraged that the 9th Circuit found AB 290 unconstitutional and unenforceable.”
Lavarn Burtonpresident and CEO of the American Kidney Foundation, called the decision “a clear victory for people with kidney failure who cannot afford health care.”
The California Department of Managed Health Care and the Department of Public Health defended the law in court, represented by the Office of the Attorney General. The departments issued a joint statement that they are “currently reviewing the decision, the impact of the decision and the appropriate next steps.”
For now, the decision leaves things as they are. Dialysis patients who currently receive premium care from the American Kidney Foundation will not see any immediate changes. But the court’s ruling leaves unresolved concerns about the overspending of dialysis care.
“I think a huge problem with the way we think about kidney care in this country is that we don’t,” Lynn said. “Although as taxpayers … we all have to think about it more than any other chronic disease because it’s so expensive.”
Supported by the California Health Care Foundation (CHCF), which works to ensure that people have access to the care they need, when they need it, at a cost they can afford. Visit www.chcf.org to learn more.
This article was originally published on CalMatters and is republished under Creative Commons Attribution-NonCommercial-No Derivatives license.